Adult Acne Is An Inside Job – Find Out Real Root-Causes
If you’re breaking out in your 30s, 40s or beyond and nothing has worked, the answer isn’t on your skin — it’s inside your body. Here’s what’s really driving it.
By Natalie Maibenko · Functional Medicine & Skincare Practitioner

You made it through your teenage years with barely a blemish. You assumed acne was behind you. And then — somewhere in your late 30s or 40s — your skin started doing something it had never done before.
Breakouts along your jaw. Cysts that take weeks to resolve. A complexion that feels inflamed, reactive, and completely unfamiliar. You’ve tried the prescriptions. Maybe antibiotics, spironolactone, even birth control pills. You’ve overhauled your skincare routine. You’ve eliminated foods, changed your pillowcase, bought every serum the internet recommended.
And still. The acne keeps coming back.
“Adult acne isn’t a skincare failure. It’s your body asking for help navigating one of the most significant hormonal transitions of your life.”
I see this every single week in my practice. Women who are intelligent, health-conscious, and deeply frustrated — not because they haven’t tried hard enough, but because everything they’ve been given treats the surface of a problem that lives much deeper.
This post is going to show you what functional medicine sees when it looks at adult acne. Not just the skin — but the hormones, the gut, the toxins, the nutrients, and the interconnected systems underneath. Because when you understand what’s actually driving your breakouts, the path forward becomes much clearer.
Why Adult Acne in Your 30s and 40s Is Different
Teenage acne and adult acne are not the same condition. Teenage acne is largely driven by a surge in androgens during puberty — a predictable, temporary hormonal shift. Adult acne, particularly in women entering perimenopause, is something altogether different.
As you approach perimenopause — which can begin as early as your mid-30s — progesterone begins to decline first. Estrogen follows, but erratically, fluctuating wildly before it finally settles into lower levels. This hormonal turbulence creates a state I describe to my patients as hormonal havoc: a period when the body is genuinely asking for help finding a new equilibrium.
During this transition, androgens (like testosterone and DHT) can become relatively dominant — even if they’re not technically elevated on a standard lab test. The ratio matters as much as the absolute number. This relative androgen excess stimulates sebaceous glands, increases sebum production, and creates the environment where acne thrives.
But here’s what almost no one tells you: the hormonal imbalance is rarely the root cause. It’s usually a downstream consequence of several other upstream problems — and that’s exactly where conventional dermatology stops looking.
What Conventional Medicine Gets Wrong About Adult Acne
I want to be clear: dermatologists are not the enemy. They are excellent at what they do. But their toolkit is designed to suppress the symptom — not investigate its origin.
Here is what I see happen, repeatedly, to the women who find their way to my practice:
Antibiotics
Prescribed to reduce the bacterial load driving breakouts. Short-term, they sometimes help. Long-term, they devastate the gut microbiome — creating dysbiosis that triggers intestinal permeability (leaky gut), malabsorption of nutrients, systemic inflammation, elevated stress hormones, higher blood sugar, and ultimately more hormonal disruption. The very thing that was meant to clear your skin ends up feeding the underlying fire.
Birth Control Pills
BCPs increase sex hormone binding globulin (SHBG), which binds free testosterone and can reduce androgen-driven acne. For some women, this works — temporarily. But BCPs also contribute to leaky gut, impair bile function, reducing absorption of fat-soluble vitamins and depleting key nutrients that are clinically linked to acne formation. When you come off the pill, the rebound can be significant.
Spironolactone
A potassium-sparing diuretic repurposed as an anti-androgen for acne. It can be effective for some patients. But for women with adrenal insufficiency — which I see frequently alongside adult acne — it can worsen exhaustion and fatigue without addressing a single root cause.
Accutane (Isotretinoin)
The nuclear option. For severe cystic acne, it can be life-changing but at the high cost. It comes with a significant burden and side effects: cheilitis, xerodermia, facial erythema, pruritis, hair thinning, brittle nails, documented risks of depression and mood disruption, liver stress with elevated enzymes, and — less commonly discussed — a measurable temporary reduction in dermal thickness and stratum corneum integrity, and even hyperpigmentation. In other words, it can create a new set of skin and health problems while clearing the old ones.
THE CORE PROBLEM: None of these approaches ask why the hormonal imbalance exists. None of them investigate what’s driving the inflammation, the sebum overproduction, the bacterial overgrowth. They manage the symptom — and for many women, that management is temporary at best.
The Real Root Causes: What I Actually Find on Your Labs
When a new patient comes to me with adult acne, I don’t start with her skin. I start with a comprehensive intake — her full history, her symptoms across every body system, and a targeted diagnostic panel. What I find, consistently, is a web of interconnected imbalances. Here are the most common findings:
Hormone Dysregulation
Elevated DHT or dihydrotestosterone (the most potent androgen), sometimes even in the presence of lower testosterone, estrogen dominance, and low progesterone are present in the majority of my adult acne patients. But I look beyond standard hormone panels — I want to see how hormones are being metabolized, which liver pathways are used in estrogen metabolism, whether there’s an increase in 5 alpha reductase enzyme activity which is responsible for testosterone conversion into DHT, whether the estrobolome (the gut bacteria responsible for estrogen processing) is functioning properly.
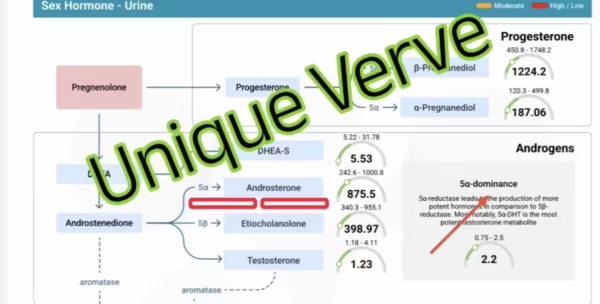
Insulin Resistance and Elevated Insulin
High insulin is one of the most direct drivers of androgen production. It stimulates the ovaries and adrenal glands to produce more androgens, which then stimulates more sebum. But elevated insulin is itself a downstream consequence — of poor sleep, gut dysbiosis, chronic stress, toxic burden and other physiological stressors. You have to follow the chain.
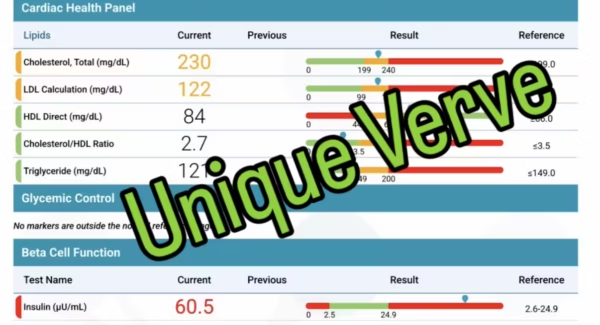
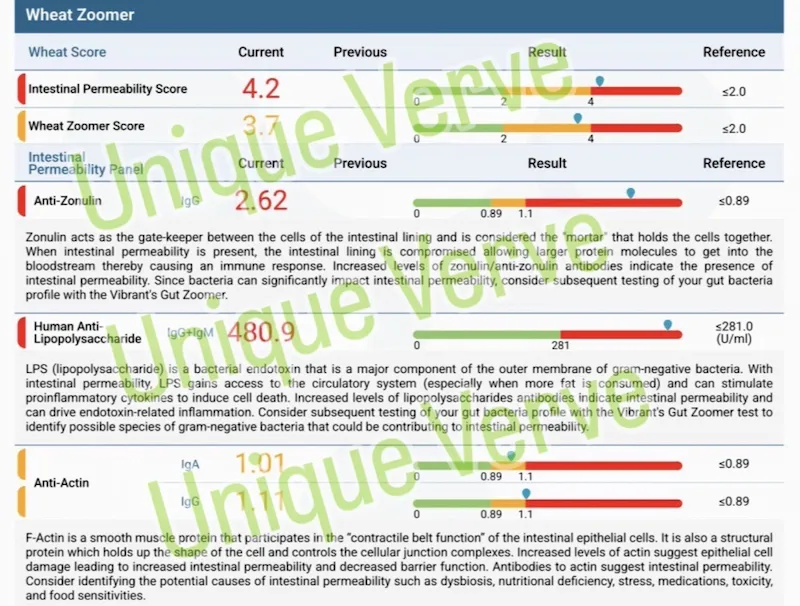
Gut Dysbiosis and Intestinal Permeability
The gut-skin axis is not a metaphor. It is a well-documented physiological relationship. When the microbiome is disrupted — by antibiotics, poor diet, stress, or infections — the intestinal lining becomes permeable. Lipopolysaccharides (bacterial endotoxins) enter the bloodstream, triggering the inflammatory cascade that shows up on your face. Meanwhile, nutrient absorption suffers, amplifying deficiencies that worsen acne.
This is the root cause that surprises my patients most.
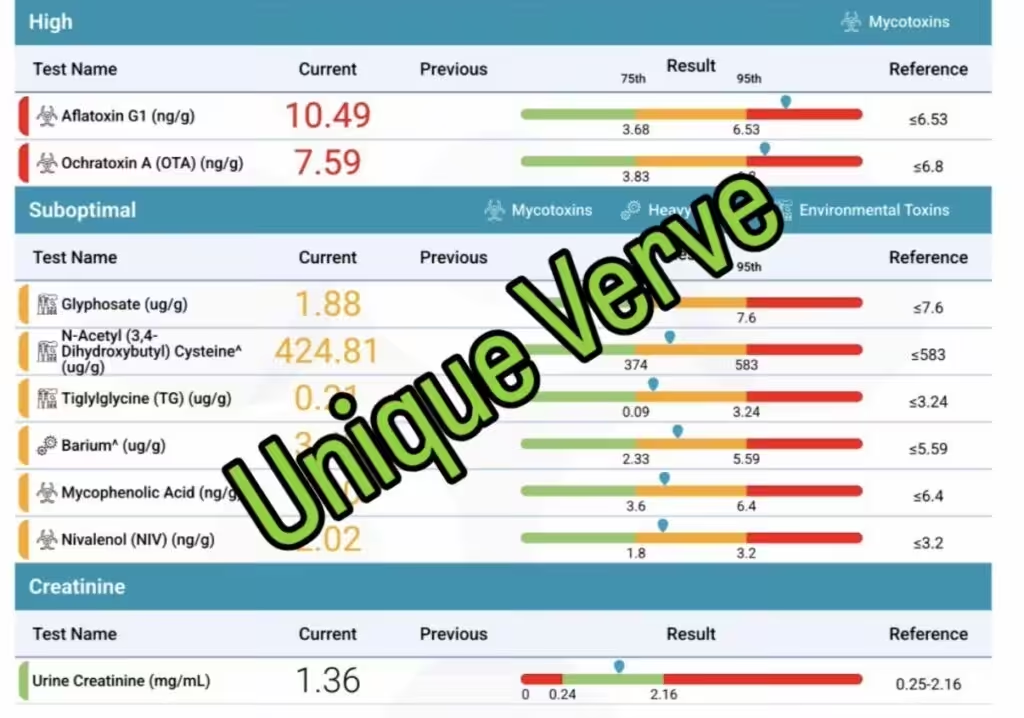
Mycotoxins, Heavy Metals, and Environmental Toxins
This is another root cause that surprises my patients — and the one most completely overlooked in conventional dermatology. Whenever I run a Total Tox Burden panel, I almost always find elevated mycotoxins (from mold exposure), heavy metals, or environmental toxins like xenoestrogens and xenoandrogens. These endocrine disruptors interfere with hormone signaling, impair liver detoxification pathways, and can directly contribute to adult acne or hormonal acne. Your environment is affecting your skin in ways your dermatologist has never tested for.
Subclinical Hypothyroidism
The thyroid connection to acne is underappreciated. Suboptimal thyroid function slows cellular turnover, impairs detoxification, and contributes to the metabolic dysfunction that drives insulin resistance. A standard TSH alone won’t capture this — you need a full thyroid panel including free T3, free T4, reverse T3 and both anti-bodies.
Nutrient Insufficiencies
Vitamin A, zinc, vitamin D, and vitamin C are all clinically associated with acne formation and/or severity of acne — yet are among the most common insufficiencies I find on micronutrient panels. Vitamin A regulates keratinocyte turnover and sebum production (it’s literally what Accutane is derived from) but without toxic side effects. Zinc prevents testosterone conversion to DHT. Vitamin D modulates immune response and lower levels are negatively associated with inflammatory lesions.
You cannot supplement your way out of deficiency without first knowing what’s actually depleted — and why.
A Real Patient Story: When Everything Had Already Been Tried
A woman came to me in her early 40s. For two years she had been dealing with persistent acne alongside a constellation of other symptoms: bloating, brain fog, profound fatigue, unexplained weight gain, hair loss, worsening allergies, and joint and muscle pain. She had been through the full conventional dermatology protocol — spironolactone, antibiotics, birth control pills, and benzoyl peroxide — without sustainable results.
When we ran her panels, the picture became clear: androgen and estrogen dominance, low progesterone, insulin resistance, gut dysbiosis, subclinical hypothyroidism, elevated mycotoxins, heavy metals, environmental toxin burden, and multiple nutrient insufficiencies including vitamin A, zinc, and vitamin D — all confirmed and cross-referenced against her genetic SNPs via a Micronutrient panel.
Her protocol addressed each layer systematically:
- Insulin Resistance— Reversed with Omega3 BioPure and Inositol, alongside dietary changes targeting the upstream physiological stressors driving pancreatic overload.
- Gut Microbiome— Rebuilt with Probiotic Integrum and Immune26 to support passive immune function and butyrate production — the short-chain fatty acid that heals the intestinal lining and improve insulin sensitivity.
- Detoxification— Supported with Liver Guard and my functional medicine detox program, specifically targeting biotransformation of mycotoxins, heavy metals, and environmental toxins.
- Nutrient Optimization— Addressed based on her specific deficiencies and SNPs: EssentialA for vitamin A, Essential Zinc, vitamin D, and additional targeted nutrients.
- Sleep and Cortisol— Prioritized with IdealMag (containing magnesium malate, L-threonate, and glycinate) to lower cortisol, promote detoxification, and support hormonal balance overnight.
- Topical Skincare— Introduced alongside internal healing with a customized Environ protocol (see below).
Within the first month, she reported incremental but meaningful improvements — more energy, less bloating, better sleep. Her skin began visibly clearing over the following two to three months as the internal work took hold. The acne that had resisted two years of pharmaceutical intervention resolved when we addressed what was actually driving it.
Ready to Find Your Root Cause?
Stop guessing. Start Testing.
Your acne has a story. A Comprehensive Functional Medicine Intake is where we read it together — and map a protocol that’s built entirely around your biology.
Diet, Lifestyle, and the Changes That Actually Move the Needle
I always test before I eliminate. Food sensitivity testing — including a Comprehensive Food Sensitivity Panel and Wheat Zoomer — tells us objectively which foods are driving an immune response, rather than asking you to follow a generic elimination diet that may or may not be relevant to your biology.
That said, there are patterns I see repeatedly across my adult acne patients:
The Common Dietary Drivers
Dairy, gluten, alcohol, and sugar are the most consistent triggers — but not universally. Dairy contains bioactive hormones and growth factors that stimulate sebum. High-glycemic foods spike insulin, which drives androgen production. Alcohol burdens the liver at the exact moment we’re trying to support detoxification. Gluten, for those with sensitivity, perpetuates intestinal permeability and also increases blood sugar and insulin as a consequence.
The key is knowing which of these applies to you — which is exactly what testing reveals.
Sleep as a Clinical Priority
Sleep is not a lifestyle suggestion. It is a biological requirement for cortisol regulation, hormonal balance, immune function and cellular detoxification. When sleep is disrupted, cortisol rises — which raises blood sugar, raises insulin, raises androgens, and drives sebum production. It is a direct pathway from poor sleep to acne.
I prioritize sleep optimization with IdealMag, which combines three forms of magnesium for synergistic effect: magnesium malate for energy metabolism, L-threonate for brain and nervous system support, and glycinate for deep relaxation and cortisol reduction. Most people are deficient in magnesium without knowing it — and this single intervention often produces the most immediate improvements in how patients feel.
The Skin Itself: Why Topicals Alone Will Never Be Enough — But They Matter
Here is something I tell every acne patient: topical skincare can produce dramatically faster visible results when the internal work is happening simultaneously. But topicals alone (just like medications), without addressing the internal drivers, is like mopping the floor with the tap still running.
Most acne patients arrive at my practice with a significantly compromised skin barrier. Years of harsh treatments — benzoyl peroxide, retinoids, exfoliating acids — have stripped the acid mantle and left the skin sensitized, reactive, and paradoxically inflamed. My first priority is always restoration, not aggression.
My Environ Protocol for Adult Acne
I treat acne-prone skin as sensitive skin first. My typical starting protocol:
Dual Action Pre-Cleansing Oil
Dissolves makeup and impurities without stripping the acid mantle
Botanical Infused Sebu-Wash Gel Cleanser
Gentle cleansing specifically formulated for acne-prone skin
Vita-Botanical Sebu-ACE Oil + Vita-Botanical Sebu-Lac Lotion
Combined to control sebum and reduce microbial overgrowth
Vita-Enriched Antioxidant Gel
Calms, soothes, and reduces inflammatory activity
Environ SPF 30
Non-negotiable for preventing post-inflammatory hyperpigmentation from the breakouts
This protocol is a starting point. As the internal healing progresses and the skin barrier rebuilds, I adjust — introducing vitamin A stepwise, adding targeted actives, and calibrating based on how the skin responds. The protocol evolves with the patient.
I use Environ exclusively for my acne patients and other inflammatory skin conditions because of its commitment to evidence-based formulation, its vitamin A philosophy, and its understanding that skin health is inseparable from skin barrier integrity. It aligns completely with my clinical approach and philosophy.
Also Recommended: If you’ve been exploring PCOS as a possible driver of your acne, read my related post: What Is the Root Cause of PCOS? Why Conventional Treatments Often Fall Short. The hormonal overlap between PCOS and perimenopausal acne is significant — and the diagnostic approach shares many of the same starting points.
Realistic Expectations: How Long Does This Take?
I will be honest with you, because I think you deserve honesty more than you need a promise.
This approach works. But it is not a prescription that clears your skin in two weeks. It is a systematic process of identifying what’s driving your acne — which is unique to you — and then methodically addressing each layer. The timeline reflects that reality.
Here is what I typically see in patients who commit fully to the protocol:
- Within the first month— Most patients notice incremental but meaningful improvements in how they feel: better energy, reduced bloating, improved GI health and sleep, more stable mood, reduction in inflammation. These systemic improvements are the foundation. Skin changes begin, but are subtle.
- Months 1–2— Visible skin improvements begin to emerge as the internal work accumulates. Inflammation reduces. New breakouts become less frequent and less severe. The skin starts to feel calmer.
- Months 2–4+— Sustained, visible clearing. This is where patients who have followed all recommendations — dietary, lifestyle, supplementation, and topical at home-treatments combined with results-oriented clinical skincare treatments — see the most significant transformation. Post-inflammatory pigmentation begins to fade. The skin barrier strengthens.
The patients who see the fastest and most sustained results are those who trust the roadmap from the beginning. This is not passive treatment — it requires active participation. But for women who have been through years of treatments that didn’t work, the relief of finally understanding and addressing the actual cause is itself transformative.
Frequently Asked Questions About Adult Acne
Why am I getting acne in my 40s when I never had it as a teenager?
Adult acne in your 30s and 40s is driven by a completely different set of factors than teenage acne. As you approach perimenopause, progesterone begins to decline first, creating a state of relative androgen excess that stimulates sebum production. This hormonal shift is also compounded by years of accumulated factors — gut dysbiosis, toxin burden, nutrient insufficiencies, insulin resistance — that were building quietly below the surface. The sudden appearance of acne is your body signaling that the system needs support.
Can birth control pills cause adult acne?
Birth control pills can both suppress and trigger acne depending on the individual and the formulation. While BCPs increase SHBG (which binds free testosterone and can reduce androgen-driven acne), they also contribute to gut permeability, impair bile function, and deplete nutrients like vitamins A, D, B6, B12, zinc, and magnesium — all of which are clinically associated with acne. Many women also experience a significant acne rebound when they stop BCPs. If you’re concerned about how BCPs may be affecting your skin, comprehensive hormone and micronutrient testing can clarify the picture.
What is the connection between gut health and acne?
The gut-skin axis is a well-documented physiological relationship. When the gut microbiome is disrupted — through antibiotics, poor diet, stress, infections or toxins — the intestinal lining can become permeable (leaky gut). Bacterial endotoxins (LPS) enter the bloodstream, triggering systemic inflammation that manifests in the skin as acne, redness, and reactivity. Simultaneously, impaired gut function reduces absorption of nutrients critical for skin health. Addressing gut dysbiosis and intestinal permeability is often one of the most impactful interventions in adult acne treatment.
How do toxins and environmental chemicals affect acne?
Mycotoxins (from mold exposure), heavy metals, xenoestrogens, and xenoandrogens (synthetic chemicals that mimic hormones) are among the most underappreciated drivers of adult acne. These endocrine disruptors interfere with hormone signaling, impair the liver’s detoxification pathways, and directly dysregulate sebum production. When I run a Total Tox Burden panel on my adult acne clients, I find elevated toxin burden in the vast majority of cases. This is a root cause that conventional dermatology never tests for — and addressing it is often transformative.
How long does a functional medicine approach to acne take to work?
Clients who follow all protocol recommendations — dietary, lifestyle, supplementation, and topical skincare — typically begin noticing systemic improvements (energy, digestion, sleep) within the first month. Visible skin improvements usually begin emerging between months one and two, with significant and sustained clearing occurring between months two and four. The timeline depends on the complexity of the individual case and the patient’s commitment to the full protocol. This is not a quick fix — it is a systematic resolution of the underlying causes.
Why do you treat adult acne skin as sensitive skin?
Most adult acne patients arrive with a compromised skin barrier — the result of years of harsh topical treatments, over-exfoliation, and prescription actives that were applied without addressing the underlying inflammation driving the acne. Restoring the acid mantle and calming the skin is the necessary first step before any targeted active ingredients are introduced. Skipping this step is one of the most common reasons topical acne treatments fail.
You have spent years looking for answers. Let’s find yours.
Adult acne in your 30s and 40s is not a skin problem — it is a whole-body signal that deserves a whole-body investigation. My Adult Acne Root Cause Program begins with your Initial Functional Medicine Health and Skin Assessment, where I review your full history, symptoms, identify your specific drivers, root-causes and build a protocol that is yours alone.
Written by Natalie Maibenko – a Certified Functional Medicine Practitioner and Master Esthetician in with 22+ years of experience and founder of Unique Verve

As a Certified Functional Medicine Practitioner my Expertise Encompasses:
- Immune System: frequent illness, UTIs, yeast infections
- Allergies, Asthma
- Skin Problems: acne, cystic acne, rosacea, eczema, dermatitis, ichthyosis, psoriasis, vitiligo, melasma
- Inflammation: arthritis, rhinitis, joint & muscle pain, migraines, headaches
- Sleep Disturbunces, Insomnia
- Gut Problems: IBS/IBD, bloating, acid reflux, gas, constipation, diarrhea, parasites, fungal/yeast overgrowths
- Hormonal Imbalances: PCOS, PMS symptoms, weight problems/inability to lose weight, thyroid problems
- Hair Loss, Alopecia
- Mood Imbalances: anxiety, depression, irritability
- Metabolic Dysfunction, Insulin Resistance, Type 2 Diabetes
- Optimizing Wellness for Successful Pregnancy
- Autoimmune Conditions: Hashimoto’s thyroiditis, grave’s disease, reumatoid arthritis (RA), lupus, etc
- Bone Health: osteopenia/ osteoporosis
- Effective Anti-Aging Strategies without Injectables with the inside-out & outside-in approach
- Detoxification of Heavy Metals, Mycotoxins, Environmental Toxins
- Reversing Breast Implant Illness
- Preparation for the Explant Surgery and Optimization of Wellness & Vitality Post-Explant
With love and gratitude,
Natalie Maibenko
Functional Medicine & Skincare Expert in Boston – Helping You Take Control of Your Health and Achieve Lasting Skin Results
DISCLAIMER:
Information and content on this website is provided for educational purposes only, and is not intended to diagnose, treat and to be a substitute for the advice provided by your physician or other healthcare professional. No information offered here should be interpreted as a diagnosis of any disease, nor an attempt to treat or prevent or cure any disease or condition. If you have any concerns or questions about your health, you should always consult with a physician or other healthcare professional. Do not disregard, avoid, or delay obtaining medical or health-related advice from your healthcare professional. Always speak with your healthcare professional before taking any medications, supplements or pursuing any wellness programs. Information provided on this website does not create a doctor-patient relationship between you and any professional affiliated with this website.
