10 Insulin Resistance Symptoms in Women Most Doctors Overlook
Insulin Resistance Symptoms in Women Most Doctors Overlook
What Is Insulin Resistance?
Insulin is a hormone produced by the pancreas that helps move glucose from the bloodstream into cells to be used for energy.
When the cells becomes less responsive to insulin, the pancreas compensates by producing more insulin to maintain normal blood sugar levels. This condition is known as insulin resistance. Over time, this condition leads to high blood sugar and prediabetes. Insulin resistance precedes a type 2 diabetes diagnosis by 10 to 15 years, with some research indicating that metabolic markers (we will discuss them further in this article) may be detectable more than 20 years prior to clinical onset.
What many women do not realize is that insulin resistance can exist for years before blood glucose levels become abnormal, start to rise and contribute to hyperglycemia.
During this early stage, fasting blood sugar test may appear completely normal within reference range, even quite optimal, while insulin levels quietly rise in the background.
From a functional medicine perspective, insulin resistance is one of the most important metabolic imbalances affecting women’s hormonal health and is strongly associated with conditions such as PCOS, hormonal acne, fatigue, hair loss, PMS symptoms, fibroids and mood instability.
The image below illustrates how insulin resistance develops and how elevated insulin levels can influence metabolism, hormones, and symptoms such as PCOS and hormonal acne in women.
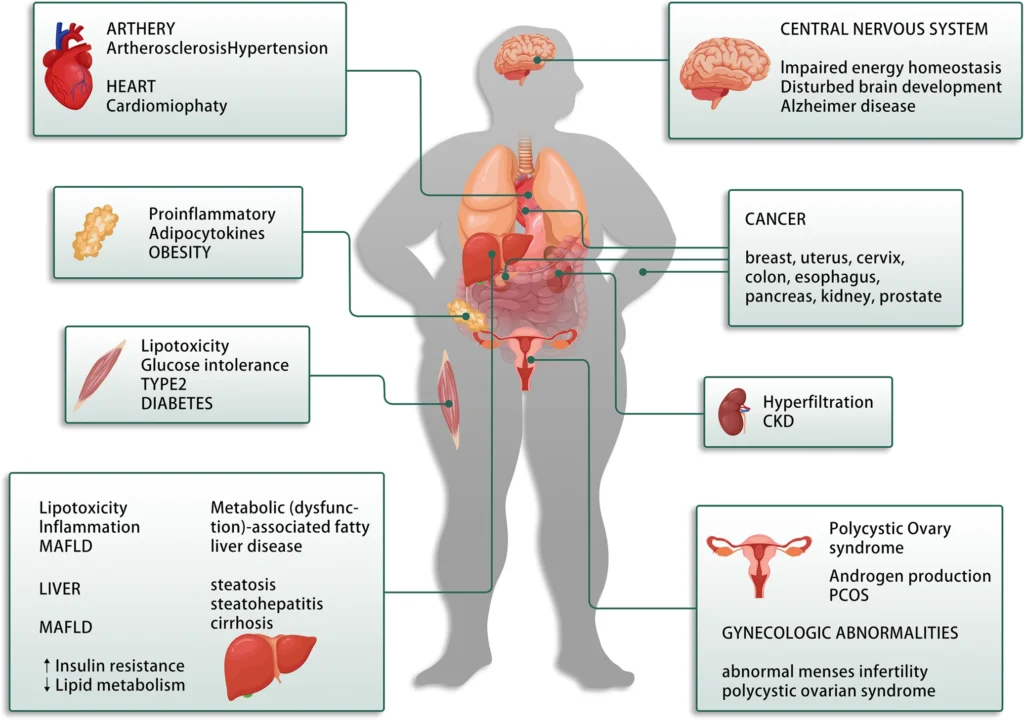
Why Insulin Resistance Often Goes Undetected
In the early stages of insulin resistance, blood glucose often remains within the normal range.
This happens because the pancreas produces increasing amounts of insulin to keep blood sugar stable.
In my clinical experience, this stage can last five to ten years before blood sugar markers begin to rise.
Unfortunately, this imbalance is frequently missed because fasting insulin is rarely tested during routine physical exams.
Many doctors evaluate only fasting glucose and/or HbA1C. If those markers appear normal, patients are often told that everything looks fine.
However, this approach can overlook the early metabolic dysfunction that may already be affecting hormonal balance, energy levels, inflammation and overall health.
The chart below shows the typical progression of insulin resistance, beginning with elevated fasting insulin while blood glucose remains normal, and eventually progressing to metabolic dysfunction.

Common Symptoms of Insulin Resistance in Women
Insulin resistance can affect many systems in the body and often presents with a wide range of symptoms.
From my clinical experience working with women, some of the most common symptoms include:
• intense sugar and carbohydrate cravings
• fatigue or lethargy
• brain fog and poor concentration
• poor memory
• mood swings or emotional sensitivity
• anxiety or panic attacks
• headaches or migraines
• chronic fatigue
• hypoglycemic episodes
• breakouts or hormonal acne
Women may also experience hormonal symptoms such as:
• irregular menstrual cycles
• heavy or prolonged menstrual bleeding
• PMS with bloating and breast tenderness
• fibrocystic breasts
• hair loss
Digestive symptoms may also be present, including:
• constipation
• bloating
• food sensitivities
Many women also report extreme emotional sensitivity, rage outbursts, or anxiety episodes, particularly when blood sugar drops.
These symptoms are often dismissed individually, yet together they can signal underlying metabolic imbalance.
The image below highlights some of the most common symptoms associated with insulin resistance in women, many of which can appear years before blood sugar levels become abnormal.

How Insulin Resistance Affects Hormones and PCOS
Insulin plays a significant role in hormone regulation.
When insulin levels are elevated, it can stimulate the ovaries to produce more androgens, including testosterone and DHT.
This hormonal shift can contribute to:
• PCOS
• hormonal acne
• irregular cycles
• fertility challenges
However, it is important not to blame hormones themselves.
Hormones are messenger molecules that respond to the body’s internal environment.
Factors such as gut health, inflammation, immune activity, detoxification pathways, toxins, thyroid function, and other metabolic hormones all influence hormonal signaling.
In functional medicine, acne and hormonal symptoms are often viewed as signals reflecting deeper imbalances within the body.
A Real Client Case: When Normal Blood Sugar Was Misleading
A 23-year-old client came to me with a wide range of symptoms she had experienced since puberty.
Her symptoms included:
• constipation
• depression and anxiety
• bloating
• chronic fatigue
• brain fog and poor memory
• intense sugar cravings
• severe PMS
• fibrocystic tender breasts
• seasonal allergies and sinus issues
• hypoglycemic episodes
• acne
• headaches
Despite these symptoms, her previous lab work had been considered normal.
Her fasting glucose was within the normal range and her HbA1C was excellent at 5.2.
However, when we evaluated fasting insulin, the results told a very different story.
Her fasting insulin measured 60.5 (reference range 2.6–24.9), indicating significant insulin resistance despite normal glucose levels.
She also had elevated LDL cholesterol and overall cholesterol levels.
The lab result below shows how elevated fasting insulin can reveal early insulin resistance even when standard blood sugar markers appear normal.
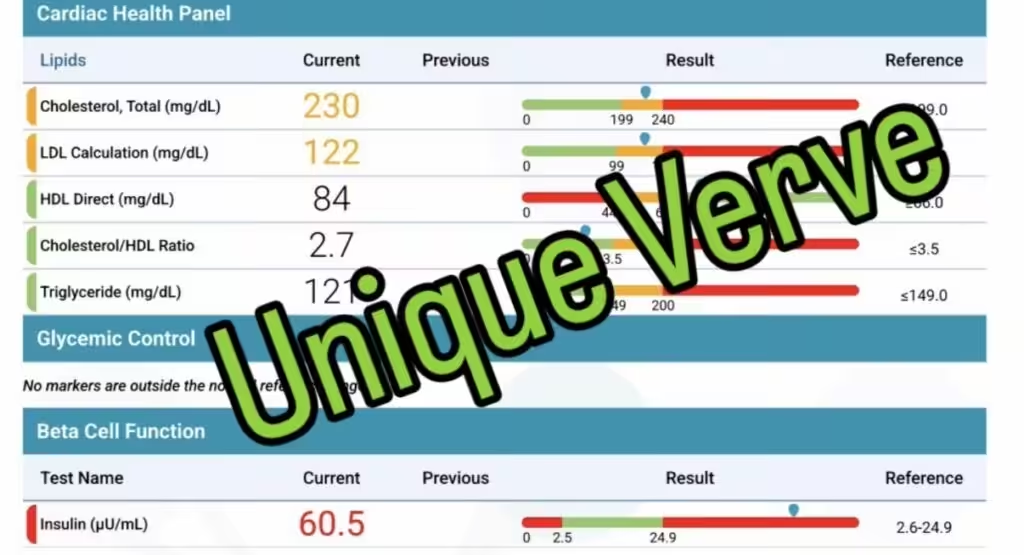
This pattern—normal glucose but elevated fasting insulin—is one of the earliest indicators of insulin resistance in women.
Further functional testing revealed high levels of mycotoxins, heavy metals, and environmental toxins, all of which are known to contribute to metabolic disruption and insulin resistance.
The test result below illustrates how environmental toxins such as mycotoxins and heavy metals can contribute to metabolic disruption and insulin resistance.
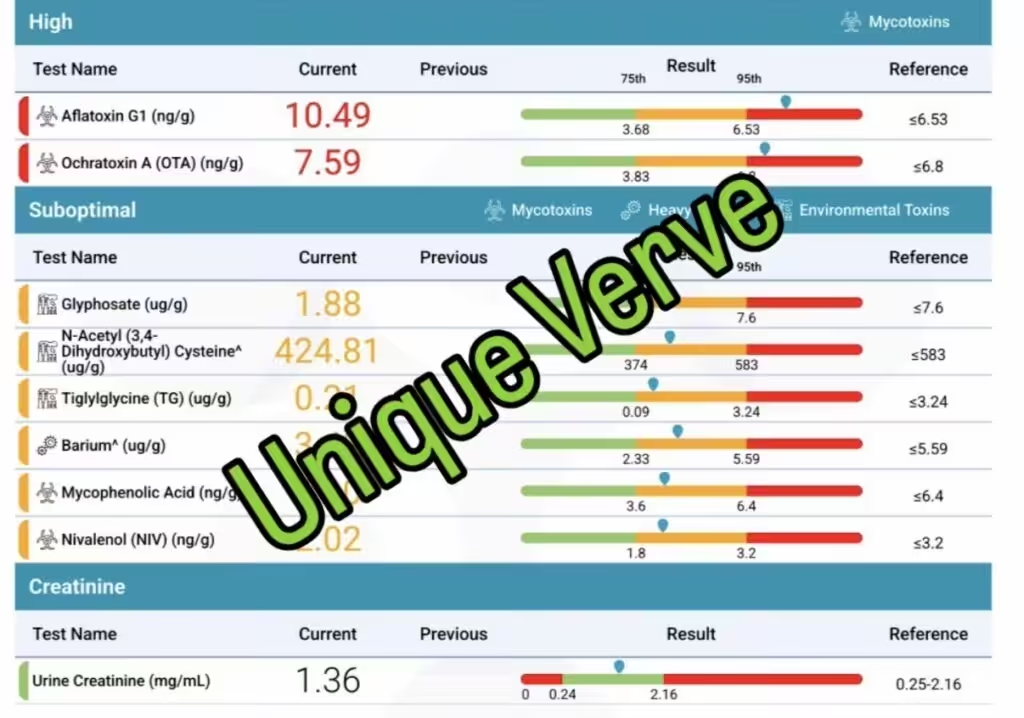
Environmental toxins can interfere with metabolic signaling and are increasingly recognized as contributors to insulin resistance.
These findings helped explain why she had been experiencing such a wide range of symptoms for many years.
Addressing the Root Causes
Once we identified the underlying contributors to her hypothyroidism, hormonal and metabolic imbalance, we implemented a personalized program that included:
• dietary and lifestyle changes
• targeted supplementation
• blood sugar stabilization strategies
• a structured detoxification protocol
Dietary strategies focused on stabilizing blood sugar by including protein, healthy fats, and leafy greens with every meal while avoiding constant snacking.
Some of the lifestyle changes included:
• morning sun exposure
• sleep optimization
• stress management
• low-impact exercise such as walking, yoga, pilates, and resistance training
Targeted nutritional supplement support for Insulin Resistance:
In addition to dietary and lifestyle interventions, targeted nutritional support can play an important role in improving insulin sensitivity and restoring metabolic balance.
However, supplements should never be viewed as a one-size-fits-all solution. In functional medicine, nutritional support is always selected based on individual symptoms, lab findings, and metabolic needs.
For example, in the case described above, several nutrients were used to support blood sugar regulation, hormone balance, and metabolic function.
These included nutrients such as inositol, which is well known for its ability to support insulin signaling and ovarian function in women, and omega-3 fatty acids, which help regulate inflammation and support metabolic health.
Additional nutrients such as zinc and B-complex vitamins may also be used when appropriate to support hormone metabolism, nervous system function, and energy production.
It is important to note that supplements work best when combined with foundational lifestyle changes, including balanced meals, stress management, proper sleep, and metabolic support strategies.
When these elements are implemented together in a personalized protocol, they can help restore metabolic balance and support the body’s ability to regulate insulin and hormone signaling and balance more effectively.
Supplement protocols should always be individualized and implemented under the guidance of a qualified practitioner.
The Transformation: What Changed Within Three Months
As we began addressing the underlying drivers and root-causes of her thyroid, hormonal and metabolic dysfunction—including insulin resistance, toxin burden, hormone imbalance, gut dysbiosis, and nutritional deficiencies—her body gradually began to rebalance.
Within three months of consistently implementing the recommended dietary, lifestyle, supplement, and detoxification strategies, the changes were remarkable.
Her cystic acne cleared, something she had struggled with since puberty. For the first time in years, her skin was no longer inflamed or painful, and she no longer felt the need to constantly search for new skincare products or treatments.
But the improvements went far beyond the skin.
Her digestive system normalized, and the chronic constipation and bloating that had been part of her daily life disappeared. She began to feel lighter and more comfortable after meals rather than sluggish and distended.
Her energy levels dramatically improved. Instead of feeling lethargic and exhausted throughout the day, she began waking up with more energy and mental clarity. The persistent brain fog that had made it difficult for her to concentrate or remember things gradually lifted.
One of the most meaningful changes for her was the improvement in her emotional well-being. The intense emotional sensitivity, anxiety, and depressive episodes that had often accompanied her cycle became far less frequent. As her blood sugar stabilized and inflammation decreased, her mood became more balanced and predictable.
Her sugar and carbohydrate cravings also disappeared, which had previously felt uncontrollable. Instead of feeling the constant urge to snack or reach for carbohydrates, she began feeling satisfied between meals.
Even symptoms she had never connected to metabolic health began to improve. Her seasonal allergies and sinus congestion became much less severe, and the headaches that had been occurring regularly diminished.
Perhaps most importantly, her PMS symptoms resolved. The heavy bleeding, painful periods, bloating, and tender fibrocystic breasts that had once made her cycle extremely difficult became significantly more manageable.
For the first time since puberty, she felt that her body was finally functioning in a balanced and stable way.
An Important Note About These Results
It is important to note that these improvements occurred because the client was fully committed to implementing the recommended changes from the beginning.
She consistently followed the dietary recommendations, incorporated the lifestyle adjustments, took the targeted supplements, and completed the detoxification protocol as recommended.
When clients actively participate in the process and address the underlying imbalances contributing to their symptoms, the body often has an incredible ability to restore balance and move toward healing.
The Body’s Capacity to Restore Balance
One of the most inspiring aspects of functional medicine is witnessing how quickly the body can begin to recover when the right conditions for healing are created.
When harmful exposures are reduced, detoxification pathways are supported, and the body is provided with the nutrients and metabolic support it needs, it often begins moving back toward homeostasis—its natural state of balance.
This case is a powerful reminder that symptoms such as acne, fatigue, brain fog, PMS, and sugar cravings are not random. They are often signals that the body is trying to communicate that something deeper is out of balance.
When those signals are investigated and addressed appropriately, meaningful improvements in health can occur.
Could These Symptoms Be Connected?
Many women are told their lab work looks “normal,” yet they continue to experience symptoms such as fatigue, brain fog, sugar cravings, PMS, acne, anxiety, or digestive issues for years without realizing that these seemingly unrelated problems may actually share a common root.
Because these symptoms often develop gradually, they are frequently normalized or treated individually rather than investigated as part of a larger pattern.
But when several of these symptoms appear together, it may be a sign that deeper metabolic or hormonal imbalances—such as insulin resistance—are present.
If you recognize yourself in this story, it may be worth taking a closer look at what your body has been trying to communicate.
A functional medicine approach looks beyond standard testing to identify early imbalances that may be affecting hormone regulation, metabolic health, and overall well-being.
Through a comprehensive health history, advanced testing, and personalized protocols, it is often possible to uncover the underlying drivers behind these symptoms and support the body in restoring balance.
Schedule a Root-Cause Consultation to explore whether insulin resistance or other metabolic factors may be contributing to your symptoms.
Frequently Asked Questions About Insulin Resistance Symptoms in Women
What are the early symptoms of insulin resistance in women?
Early symptoms of insulin resistance in women may appear years before blood sugar levels become abnormal. Common symptoms include fatigue, intense sugar cravings, brain fog, mood swings, hormonal acne, irregular menstrual cycles, PMS, headaches, and difficulty concentrating. Many women also experience hypoglycemic episodes, anxiety, or sudden drops in energy between meals.
Can insulin resistance cause hormonal acne?
Yes. Elevated insulin levels can stimulate the ovaries to produce higher amounts of androgens, including testosterone and DHT. These hormones can increase oil production in the skin and contribute to clogged pores and inflammatory acne, particularly along the chin and jawline. Insulin resistance is commonly associated with hormonal acne and conditions such as PCOS.
Why is fasting insulin important for detecting insulin resistance?
Fasting insulin can reveal metabolic dysfunction years before blood glucose or HbA1C become abnormal. In early insulin resistance, the body produces higher levels of insulin to maintain normal blood sugar levels. Because fasting insulin is not routinely tested during standard physical exams, early metabolic imbalance may go undetected if only blood glucose is evaluated.
Can insulin resistance occur even if blood sugar levels are normal?
Yes. Insulin resistance often develops long before blood glucose levels rise. During the early stages, fasting glucose and HbA1C may remain within the normal range while insulin levels increase significantly. This is why evaluating fasting insulin alongside glucose and HbA1C can provide a more complete picture of metabolic health.
What conditions are commonly linked to insulin resistance in women?
Insulin resistance in women is associated with several health conditions, including PCOS, hormonal acne, hypothyroidism, irregular menstrual cycles, infertility, metabolic syndrome, and non-alcoholic fatty liver disease. It may also contribute to symptoms such as fatigue, sugar cravings, mood changes, and difficulty losing weight.
Can lifestyle changes improve insulin resistance?
Yes. Dietary changes that stabilize blood sugar, adequate protein and healthy fats with meals, regular physical activity, stress management, and sufficient sleep can significantly improve insulin sensitivity. Targeted nutritional support and addressing underlying factors such as toxin exposure or nutrient deficiencies may also help restore metabolic balance.
When should someone consider testing for insulin resistance?
If you experience symptoms such as fatigue, sugar cravings, hormonal acne, PMS symptoms, brain fog, anxiety, or irregular cycles despite normal routine lab results, it may be helpful to evaluate deeper metabolic markers such as fasting insulin, fasting glucose, and HbA1C together.
Written by Natalie Maibenko – a Certified Functional Medicine Practitioner and Licensed Esthetician in Boston with 22+ years of experience and founder of Unique Verve

Natalie Maibenko
Functional Medicine & Skincare Expert in Boston – Helping You Take Control of Your Health and Achieve Lasting Skin Results
As a Certified Functional Medicine Practitioner my Expertise Encompasses:
- Immune System: frequent illness, UTIs, yeast infections
- Allergies, Asthma
- Skin Problems: acne, cystic acne, rosacea, eczema, dermatitis, ichthyosis, psoriasis, vitiligo, melasma
- Inflammation: arthritis, rhinitis, joint & muscle pain, migraines, headaches
- Sleep Disturbunces, Insomnia
- Gut Problems: IBS/IBD, bloating, acid reflux, gas, constipation, diarrhea, parasites, fungal/yeast overgrowths
- Hormonal Imbalances: PCOS, PMS symptoms, weight problems/inability to lose weight, thyroid problems
- Hair Loss, Alopecia
- Mood Imbalances: anxiety, depression, irritability
- Metabolic Dysfunction, Insulin Resistance, Type 2 Diabetes
- Optimizing Wellness for Successful Pregnancy
- Autoimmune Conditions: Hashimoto’s thyroiditis, grave’s disease, reumatoid arthritis (RA), lupus, etc
- Bone Health: osteopenia/ osteoporosis
- Effective Anti-Aging Strategies without Injectables with the inside-out & outside-in approach
- Detoxification of Heavy Metals, Mycotoxins, Environmental Toxins
- Reversing Breast Implant Illness
- Preparation for the Explant Surgery and Optimization of Wellness & Vitality Post-Explant
DISCLAIMER:
Information and content on this website is provided for educational purposes only, and is not intended to diagnose, treat and to be a substitute for the advice provided by your physician or other healthcare professional. No information offered here should be interpreted as a diagnosis of any disease, nor an attempt to treat or prevent or cure any disease or condition. If you have any concerns or questions about your health, you should always consult with a physician or other healthcare professional. Do not disregard, avoid, or delay obtaining medical or health-related advice from your healthcare professional. Always speak with your healthcare professional before taking any medications, supplements or pursuing any wellness programs. Information provided on this website does not create a doctor-patient relationship between you and any professional affiliated with this website.
